Life Expectancy vs. Healthcare Spending Across the World’s Top Economies
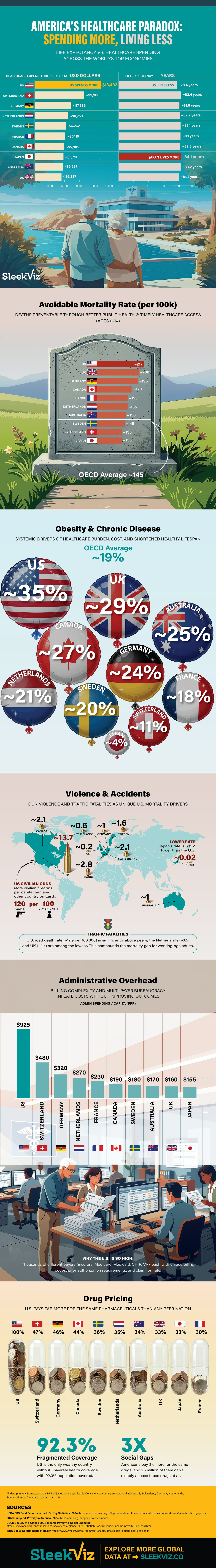
The United States spends more money on healthcare than any other country on Earth. Not by a little. By a lot. In 2023, Americans spent an estimated $13,432 per person on healthcare. That is nearly double what Germany spends, almost triple what Japan spends, and more than $3,500 above the next highest spender, Switzerland.
You would expect that kind of investment to produce extraordinary results. Longer lives, healthier populations, world-leading outcomes. And in some specific areas of medicine, it does. American hospitals perform cutting-edge surgeries. American pharmaceutical companies develop drugs that the rest of the world eventually adopts. American medical research drives global innovation.
But when you zoom out and look at the most basic measure of a health system’s success, how long its people actually live, the United States falls behind every single one of its wealthy peers. Every one.
Life expectancy in the U.S. is 78.4 years. The comparable country average among peer nations is 82.5 years. That four-year gap represents millions of lives cut shorter than they should be, and it has been widening for decades.
This is America’s healthcare paradox.
The Numbers That Started the Conversation
To understand just how unusual the United States is, it helps to look at the data side by side.
Switzerland, the second-highest spender among wealthy nations, spends around $9,900 per person and achieves a life expectancy of roughly 83.4 years. Germany spends $7,383 and lives to about 81.6. Japan spends $5,790 and reaches 84.1 years, the highest life expectancy among the ten countries in this analysis.
Japan is worth pausing on. It spends less per person than the OECD average, operates below many of its European counterparts in raw dollars, and yet consistently tops global life expectancy rankings. Something is clearly working there that has nothing to do with spending volume.
The pattern holds across every country in this comparison. Australia, Canada, France, Sweden, the Netherlands, the United Kingdom. They all spend significantly less than the United States. They all live longer.
The relationship between money and health is not linear. At lower spending levels, additional investment in healthcare makes a dramatic difference. Countries that move from very low to moderate health spending see enormous gains in life expectancy. But once a country crosses a certain threshold of investment, around $5,000 per capita, those returns begin to flatten. The U.S. sits so far past that point that additional spending is essentially not translating into additional years of life at all.
This is what economists call diminishing returns. And the United States may be the most extreme example of it in the world.
Why Is This Happening? The Six Drivers
The gap between what America spends and what it gets in return is not a mystery. Researchers, policymakers, and public health experts have been studying it for decades. The evidence points to six interconnected factors, none of which alone explains the paradox, but together they paint a complete picture.
1. Avoidable Deaths Are Rising, Not Falling
In most wealthy countries, the number of deaths that could have been prevented through better healthcare or public health interventions has been declining steadily for years. In the United States, it has been going up.
A 2025 study published in JAMA Internal Medicine by researchers at Brown University and Harvard compared avoidable mortality trends across all 50 U.S. states and 40 high-income countries between 2009 and 2021. The findings were striking. Avoidable mortality increased in every single U.S. state over that period. In most peer countries, it decreased.
The U.S. preventable mortality rate now sits at approximately 217 deaths per 100,000 people. The OECD average is 145. Switzerland and Japan, the best performers, are both below 135. That gap, nearly 50% higher than the international average, represents an enormous number of deaths that should not be happening in the world’s highest-spending healthcare system.
The causes behind this increase are not isolated to one disease or one demographic. Deaths from drug overdoses, chronic disease complications, and suicides are all rising. And critically, so are deaths from conditions that effective healthcare systems routinely catch and treat early.
2. Obesity and Chronic Disease Are Systemic Problems
The United States has an adult obesity rate of roughly 35%. The OECD average among wealthy countries is about 19%. Japan’s rate is approximately 4%.
This is not purely a matter of individual choices. Obesity is shaped by food environments, urban design, socioeconomic stress, the availability and marketing of ultra-processed foods, and a hundred other structural factors. Countries with low obesity rates tend to have food systems, built environments, and social safety nets that make healthy choices easier and more affordable by default.
The healthcare cost of this difference is enormous. The OECD estimates that overweight and obesity add approximately $209 per capita per year to healthcare costs across member countries, and account for around 8.4% of total health budgets. For the United States, with its significantly higher obesity prevalence, the burden is proportionally larger.
Obesity drives type 2 diabetes, cardiovascular disease, certain cancers, and sleep apnea, all of which are far more prevalent in the U.S. than in peer nations and all of which require expensive, ongoing treatment. Prevention is dramatically cheaper than treatment, but prevention requires systemic investment that goes beyond the healthcare system itself.
3. Gun Violence and Accidents Are Pulling Life Expectancy Down
This is the driver that often surprises people outside the United States, but the data is unambiguous.
In 2023, approximately 46,728 people died from gun-related injuries in the United States. That translates to a total firearm death rate of 13.7 per 100,000 people. France, the peer country with the next highest rate, sits at around 2.8 per 100,000. The United Kingdom is at roughly 0.2. Japan is at 0.02.
The U.S. firearm death rate is nearly five times that of France, and almost 700 times that of Japan.
Firearms are now the leading cause of death for children and teenagers in the United States. Gun violence is disproportionately concentrated among working-age adults, which has an outsized effect on average life expectancy statistics because deaths at younger ages subtract more years from the population average than deaths at older ages.
Traffic fatalities compound the issue. The U.S. road death rate significantly exceeds those of peer nations, with countries like the Netherlands and the United Kingdom achieving rates roughly three to four times lower.
These are not healthcare system failures in the traditional sense. But they are unmistakably public health failures, and they fall heavily on the life expectancy calculation.
4. Administrative Overhead Is Consuming a Staggering Share of Healthcare Dollars
The United States spends approximately $925 per person per year on healthcare administration. The comparable country average among peer nations is around $230.
That is four times more spent on billing, insurance overhead, claims processing, and regulatory compliance, without producing a single additional unit of care.
In the U.S. system, thousands of different payers, private insurers, Medicare, Medicaid, CHIP, the VA, and many others all operate with different billing codes, prior authorization requirements, and claim formats. Hospitals and medical practices need armies of administrative staff just to navigate this complexity. One landmark study published in JAMA estimated that administrative costs account for 8% of total U.S. health spending, compared to just 1 to 3% in peer countries.
By contrast, countries with single-payer or tightly regulated insurance systems, like Canada, the UK, Japan, Australia, and Sweden, operate with dramatically lower administrative overhead. That money goes elsewhere. Toward care, toward prevention, toward personnel.
McKinsey has estimated that administrative simplification alone could save approximately $265 billion annually in the U.S. healthcare system. That is real money that is currently being spent on paperwork.
5. Americans Pay Far More for the Same Drugs
A 2024 report from RAND Health Care, commissioned by the U.S. Department of Health and Human Services, compared prescription drug prices in the United States with those in 33 other OECD countries using 2022 data.
The results were remarkable. U.S. prices for all drugs, brands and generics combined, were 2.78 times higher than the OECD average. For brand-name drugs specifically, U.S. prices were at least 3.22 times higher, even after adjusting for estimated rebates.
Insulin tells the sharpest version of this story. In 2022, U.S. insulin prices were nearly ten times higher than the OECD average. A vial of insulin that costs $10 in France costs close to $100 in the United States. For the nearly 8 million Americans who rely on insulin, this is not an abstract policy statistic. It is a monthly financial calculation that sometimes ends in rationing doses.
The reason for this gap is structural. Most wealthy countries use some form of government negotiation or reference pricing to set pharmaceutical prices. Manufacturers must justify their prices against health outcomes data or accept regulated caps. In the United States, manufacturers historically set their own prices with limited government intervention, and the market has responded accordingly.
The Inflation Reduction Act began changing this for Medicare in 2022, allowing the U.S. government to negotiate prices on a limited set of drugs for the first time. But the gap with peer nations remains wide.
6. A Quarter of Americans Are One Job Away from Losing Coverage
Every other country in this ten-nation comparison has achieved universal or near-universal health coverage. Germany, France, the UK, Canada, Australia, Japan, Sweden, the Netherlands, and Switzerland all cover essentially 100% of their populations through either public systems or compulsory regulated private insurance.
The United States covers approximately 92.3%. That means roughly 25.3 million Americans have no health insurance at all.
But the uninsured rate only tells part of the story. An estimated one in four insured Americans is considered underinsured, meaning their deductibles and co-payments are high enough that they delay or skip care due to cost. More than 21% of Americans report skipping prescribed medications because they cannot afford them. These are not uninsured people. These are people with coverage who still cannot access the system.
Perhaps most telling is the structural fragility of U.S. coverage. Roughly 54% of Americans get their health insurance through an employer. That means a job loss, a divorce, or a business closure can trigger an immediate loss of healthcare access. In every peer nation, coverage is tied to residency or citizenship, not employment status.
The Countries Getting It Right
It would be easy to read the above and conclude that healthcare is simply an unsolvable problem. But the data from peer nations suggests otherwise.
Japan offers the most instructive example. With a per-capita health spend below the OECD average and an obesity rate of just 4%, Japan achieves the highest life expectancy among the ten countries analyzed, at 84.1 years. Its healthy life expectancy, meaning years lived without disability, is 73.2 years, compared to 66.1 years in the United States.
Japan’s system is built on compulsory social insurance, a diet historically rich in fish and vegetables, strong primary care infrastructure, and very low rates of the lifestyle-driven chronic diseases that burden the U.S. system. It is not perfect. Japan faces demographic pressures from an aging population and a healthcare workforce that is stretched thin. But as a model of efficiency, it is hard to ignore.
Sweden shows a different path. With a Gini coefficient of 0.27, the lowest income inequality among the ten countries analyzed, and one of the highest rates of social spending as a share of GDP at 22.2%, Sweden has built an environment where the social determinants of health, housing stability, food security, income adequacy, are addressed before people need clinical care. Its child poverty rate is just 7.9%, compared to 13.7% in the United States. Its life expectancy is 83.1 years.
Switzerland is the most instructive comparison for the United States because it also uses private insurance. But Swiss insurance is compulsory, tightly regulated, and operates within a single standardized risk pool. Administrative overhead is a fraction of the U.S. equivalent. Insurers cannot refuse applicants or charge more based on health status. The result is near-universal coverage at $9,900 per capita, compared to $13,432 in the U.S., with meaningfully better health outcomes.
The 1980 Baseline
One detail in the data deserves more attention than it usually gets.
In 1980, the United States had a life expectancy and a healthcare spending level that were broadly comparable to its peer nations. The gap that exists today did not always exist. It developed over the following four decades as U.S. spending grew dramatically faster than its peers while life expectancy gains stalled and eventually reversed.
This matters because it demonstrates that the current situation is not inevitable. It is the product of specific policy choices, structural decisions, and systemic features that diverged from the paths taken by other wealthy nations. That means it is, at least in theory, reversible.
What This Means
The healthcare paradox is not a simple story about a broken system. The United States has world-class hospitals, extraordinary medical technology, and brilliant clinicians. It leads the world in pharmaceutical innovation and performs some categories of specialized care better than anywhere else.
The paradox is that none of that translates to population-level outcomes. Because outcomes are not just determined by what happens inside a hospital. They are determined by whether people can afford to go to the hospital in the first place, whether they can afford the drugs prescribed when they leave, whether they live in an environment that supports their health between visits, and whether they are likely to die from a preventable cause before they ever need a hospital at all.
Spending more is not the answer. How that money is spent, and what it is directed toward, is what separates a high-performing health system from an expensive one.
The countries at the top of the life expectancy ranking are not there because they spent their way there. They are there because they built systems where the money they do spend is directed efficiently, equitably, and preventively. The United States has not yet done that. The data makes that very clear.
Methodology Note
This analysis draws on data primarily from the OECD Health Statistics database, Peterson-KFF Health System Tracker, RAND/ASPE international drug price comparisons (2022 data, published February 2024), the CDC, WHO Global Health Observatory, USDA Economic Research Service, and the Brown University/JAMA Internal Medicine study on avoidable mortality (published March 2025). Health spending figures are expressed in PPP-adjusted U.S. dollars to account for differences in purchasing power across countries. Life expectancy and mortality figures reflect the most recent year of comparable cross-national data available, primarily 2021 to 2023 depending on the indicator. All figures are rounded. The ten countries included in this analysis are the United States, Switzerland, Germany, the Netherlands, Sweden, France, Canada, Japan, Australia, and the United Kingdom.
The United States spends more money on healthcare than any other country on Earth. Not by a little. By a lot. In 2023, Americans spent an estimated $13,432 per person on healthcare. That is nearly double what Germany spends, almost triple what Japan spends, and more than $3,500 above the next highest spender, Switzerland.
You would expect that kind of investment to produce extraordinary results. Longer lives, healthier populations, world-leading outcomes. And in some specific areas of medicine, it does. American hospitals perform cutting-edge surgeries. American pharmaceutical companies develop drugs that the rest of the world eventually adopts. American medical research drives global innovation.
But when you zoom out and look at the most basic measure of a health system’s success, how long its people actually live, the United States falls behind every single one of its wealthy peers. Every one.
Life expectancy in the U.S. is 78.4 years. The comparable country average among peer nations is 82.5 years. That four-year gap represents millions of lives cut shorter than they should be, and it has been widening for decades.
This is America’s healthcare paradox.
The Numbers That Started the Conversation
To understand just how unusual the United States is, it helps to look at the data side by side.
Switzerland, the second-highest spender among wealthy nations, spends around $9,900 per person and achieves a life expectancy of roughly 83.4 years. Germany spends $7,383 and lives to about 81.6. Japan spends $5,790 and reaches 84.1 years, the highest life expectancy among the ten countries in this analysis.
Japan is worth pausing on. It spends less per person than the OECD average, operates below many of its European counterparts in raw dollars, and yet consistently tops global life expectancy rankings. Something is clearly working there that has nothing to do with spending volume.
The pattern holds across every country in this comparison. Australia, Canada, France, Sweden, the Netherlands, the United Kingdom. They all spend significantly less than the United States. They all live longer.
The relationship between money and health is not linear. At lower spending levels, additional investment in healthcare makes a dramatic difference. Countries that move from very low to moderate health spending see enormous gains in life expectancy. But once a country crosses a certain threshold of investment, around $5,000 per capita, those returns begin to flatten. The U.S. sits so far past that point that additional spending is essentially not translating into additional years of life at all.
This is what economists call diminishing returns. And the United States may be the most extreme example of it in the world.
Why Is This Happening? The Six Drivers
The gap between what America spends and what it gets in return is not a mystery. Researchers, policymakers, and public health experts have been studying it for decades. The evidence points to six interconnected factors, none of which alone explains the paradox, but together they paint a complete picture.
1. Avoidable Deaths Are Rising, Not Falling
In most wealthy countries, the number of deaths that could have been prevented through better healthcare or public health interventions has been declining steadily for years. In the United States, it has been going up.
A 2025 study published in JAMA Internal Medicine by researchers at Brown University and Harvard compared avoidable mortality trends across all 50 U.S. states and 40 high-income countries between 2009 and 2021. The findings were striking. Avoidable mortality increased in every single U.S. state over that period. In most peer countries, it decreased.
The U.S. preventable mortality rate now sits at approximately 217 deaths per 100,000 people. The OECD average is 145. Switzerland and Japan, the best performers, are both below 135. That gap, nearly 50% higher than the international average, represents an enormous number of deaths that should not be happening in the world’s highest-spending healthcare system.
The causes behind this increase are not isolated to one disease or one demographic. Deaths from drug overdoses, chronic disease complications, and suicides are all rising. And critically, so are deaths from conditions that effective healthcare systems routinely catch and treat early.
2. Obesity and Chronic Disease Are Systemic Problems
The United States has an adult obesity rate of roughly 35%. The OECD average among wealthy countries is about 19%. Japan’s rate is approximately 4%.
This is not purely a matter of individual choices. Obesity is shaped by food environments, urban design, socioeconomic stress, the availability and marketing of ultra-processed foods, and a hundred other structural factors. Countries with low obesity rates tend to have food systems, built environments, and social safety nets that make healthy choices easier and more affordable by default.
The healthcare cost of this difference is enormous. The OECD estimates that overweight and obesity add approximately $209 per capita per year to healthcare costs across member countries, and account for around 8.4% of total health budgets. For the United States, with its significantly higher obesity prevalence, the burden is proportionally larger.
Obesity drives type 2 diabetes, cardiovascular disease, certain cancers, and sleep apnea, all of which are far more prevalent in the U.S. than in peer nations and all of which require expensive, ongoing treatment. Prevention is dramatically cheaper than treatment, but prevention requires systemic investment that goes beyond the healthcare system itself.
3. Gun Violence and Accidents Are Pulling Life Expectancy Down
This is the driver that often surprises people outside the United States, but the data is unambiguous.
In 2023, approximately 46,728 people died from gun-related injuries in the United States. That translates to a total firearm death rate of 13.7 per 100,000 people. France, the peer country with the next highest rate, sits at around 2.8 per 100,000. The United Kingdom is at roughly 0.2. Japan is at 0.02.
The U.S. firearm death rate is nearly five times that of France, and almost 700 times that of Japan.
Firearms are now the leading cause of death for children and teenagers in the United States. Gun violence is disproportionately concentrated among working-age adults, which has an outsized effect on average life expectancy statistics because deaths at younger ages subtract more years from the population average than deaths at older ages.
Traffic fatalities compound the issue. The U.S. road death rate significantly exceeds those of peer nations, with countries like the Netherlands and the United Kingdom achieving rates roughly three to four times lower.
These are not healthcare system failures in the traditional sense. But they are unmistakably public health failures, and they fall heavily on the life expectancy calculation.
4. Administrative Overhead Is Consuming a Staggering Share of Healthcare Dollars
The United States spends approximately $925 per person per year on healthcare administration. The comparable country average among peer nations is around $230.
That is four times more spent on billing, insurance overhead, claims processing, and regulatory compliance, without producing a single additional unit of care.
In the U.S. system, thousands of different payers, private insurers, Medicare, Medicaid, CHIP, the VA, and many others all operate with different billing codes, prior authorization requirements, and claim formats. Hospitals and medical practices need armies of administrative staff just to navigate this complexity. One landmark study published in JAMA estimated that administrative costs account for 8% of total U.S. health spending, compared to just 1 to 3% in peer countries.
By contrast, countries with single-payer or tightly regulated insurance systems, like Canada, the UK, Japan, Australia, and Sweden, operate with dramatically lower administrative overhead. That money goes elsewhere. Toward care, toward prevention, toward personnel.
McKinsey has estimated that administrative simplification alone could save approximately $265 billion annually in the U.S. healthcare system. That is real money that is currently being spent on paperwork.
5. Americans Pay Far More for the Same Drugs
A 2024 report from RAND Health Care, commissioned by the U.S. Department of Health and Human Services, compared prescription drug prices in the United States with those in 33 other OECD countries using 2022 data.
The results were remarkable. U.S. prices for all drugs, brands and generics combined, were 2.78 times higher than the OECD average. For brand-name drugs specifically, U.S. prices were at least 3.22 times higher, even after adjusting for estimated rebates.
Insulin tells the sharpest version of this story. In 2022, U.S. insulin prices were nearly ten times higher than the OECD average. A vial of insulin that costs $10 in France costs close to $100 in the United States. For the nearly 8 million Americans who rely on insulin, this is not an abstract policy statistic. It is a monthly financial calculation that sometimes ends in rationing doses.
The reason for this gap is structural. Most wealthy countries use some form of government negotiation or reference pricing to set pharmaceutical prices. Manufacturers must justify their prices against health outcomes data or accept regulated caps. In the United States, manufacturers historically set their own prices with limited government intervention, and the market has responded accordingly.
The Inflation Reduction Act began changing this for Medicare in 2022, allowing the U.S. government to negotiate prices on a limited set of drugs for the first time. But the gap with peer nations remains wide.
6. A Quarter of Americans Are One Job Away from Losing Coverage
Every other country in this ten-nation comparison has achieved universal or near-universal health coverage. Germany, France, the UK, Canada, Australia, Japan, Sweden, the Netherlands, and Switzerland all cover essentially 100% of their populations through either public systems or compulsory regulated private insurance.
The United States covers approximately 92.3%. That means roughly 25.3 million Americans have no health insurance at all.
But the uninsured rate only tells part of the story. An estimated one in four insured Americans is considered underinsured, meaning their deductibles and co-payments are high enough that they delay or skip care due to cost. More than 21% of Americans report skipping prescribed medications because they cannot afford them. These are not uninsured people. These are people with coverage who still cannot access the system.
Perhaps most telling is the structural fragility of U.S. coverage. Roughly 54% of Americans get their health insurance through an employer. That means a job loss, a divorce, or a business closure can trigger an immediate loss of healthcare access. In every peer nation, coverage is tied to residency or citizenship, not employment status.
The Countries Getting It Right
It would be easy to read the above and conclude that healthcare is simply an unsolvable problem. But the data from peer nations suggests otherwise.
Japan offers the most instructive example. With a per-capita health spend below the OECD average and an obesity rate of just 4%, Japan achieves the highest life expectancy among the ten countries analyzed, at 84.1 years. Its healthy life expectancy, meaning years lived without disability, is 73.2 years, compared to 66.1 years in the United States.
Japan’s system is built on compulsory social insurance, a diet historically rich in fish and vegetables, strong primary care infrastructure, and very low rates of the lifestyle-driven chronic diseases that burden the U.S. system. It is not perfect. Japan faces demographic pressures from an aging population and a healthcare workforce that is stretched thin. But as a model of efficiency, it is hard to ignore.
Sweden shows a different path. With a Gini coefficient of 0.27, the lowest income inequality among the ten countries analyzed, and one of the highest rates of social spending as a share of GDP at 22.2%, Sweden has built an environment where the social determinants of health, housing stability, food security, income adequacy, are addressed before people need clinical care. Its child poverty rate is just 7.9%, compared to 13.7% in the United States. Its life expectancy is 83.1 years.
Switzerland is the most instructive comparison for the United States because it also uses private insurance. But Swiss insurance is compulsory, tightly regulated, and operates within a single standardized risk pool. Administrative overhead is a fraction of the U.S. equivalent. Insurers cannot refuse applicants or charge more based on health status. The result is near-universal coverage at $9,900 per capita, compared to $13,432 in the U.S., with meaningfully better health outcomes.
The 1980 Baseline
One detail in the data deserves more attention than it usually gets.
In 1980, the United States had a life expectancy and a healthcare spending level that were broadly comparable to its peer nations. The gap that exists today did not always exist. It developed over the following four decades as U.S. spending grew dramatically faster than its peers while life expectancy gains stalled and eventually reversed.
This matters because it demonstrates that the current situation is not inevitable. It is the product of specific policy choices, structural decisions, and systemic features that diverged from the paths taken by other wealthy nations. That means it is, at least in theory, reversible.
What This Means
The healthcare paradox is not a simple story about a broken system. The United States has world-class hospitals, extraordinary medical technology, and brilliant clinicians. It leads the world in pharmaceutical innovation and performs some categories of specialized care better than anywhere else.
The paradox is that none of that translates to population-level outcomes. Because outcomes are not just determined by what happens inside a hospital. They are determined by whether people can afford to go to the hospital in the first place, whether they can afford the drugs prescribed when they leave, whether they live in an environment that supports their health between visits, and whether they are likely to die from a preventable cause before they ever need a hospital at all.
Spending more is not the answer. How that money is spent, and what it is directed toward, is what separates a high-performing health system from an expensive one.
The countries at the top of the life expectancy ranking are not there because they spent their way there. They are there because they built systems where the money they do spend is directed efficiently, equitably, and preventively. The United States has not yet done that. The data makes that very clear.
Methodology Note
This analysis draws on data primarily from the OECD Health Statistics database, Peterson-KFF Health System Tracker, RAND/ASPE international drug price comparisons (2022 data, published February 2024), the CDC, WHO Global Health Observatory, USDA Economic Research Service, and the Brown University/JAMA Internal Medicine study on avoidable mortality (published March 2025). Health spending figures are expressed in PPP-adjusted U.S. dollars to account for differences in purchasing power across countries. Life expectancy and mortality figures reflect the most recent year of comparable cross-national data available, primarily 2021 to 2023 depending on the indicator. All figures are rounded. The ten countries included in this analysis are the United States, Switzerland, Germany, the Netherlands, Sweden, France, Canada, Japan, Australia, and the United Kingdom.
Sources & Citations
1. Peterson-KFF Health System Tracker — “How does U.S. life expectancy compare to other countries?” (Jan. 2025) — https://www.healthsystemtracker.org/chart-collection/u-s-life-expectancy-compare-countries/
2. Peterson-KFF Health System Tracker — “How does health spending in the U.S. compare to other countries?” (Apr. 2025) — https://www.healthsystemtracker.org/chart-collection/health-spending-u-s-compare-countries/
3. OECD — Health at a Glance 2023 — https://www.oecd.org/en/publications/health-at-a-glance-2023_7a7afb35-en.html
4. OECD — Health at a Glance 2025 (Japan Country Note) — https://www.oecd.org/en/publications/health-at-a-glance-2025_15a55280-en/japan_319bfc39-en.html
5. Our World in Data — Healthcare Spending & Life Expectancy — https://ourworldindata.org/financing-healthcare
6. World Economic Forum — “Here’s how countries compare on healthcare expenditure and life expectancy” — https://www.weforum.org/stories/2022/11/countries-compare-on-healthcare-expenditure-life-expectancy/
7. World Population Review — Healthcare Spending by Country — https://worldpopulationreview.com/country-rankings/healthcare-spending-by-country
8. WHO Global Health Observatory — Healthy Life Expectancy (HALE) — https://www.who.int/data/gho/data/themes/mortality-and-global-health-estimates/ghe-life-expectancy-and-healthy-life-expectancy
9. OECD Health at a Glance 2025 — Avoidable Mortality & Obesity Data — https://www.oecd.org/en/publications/health-at-a-glance-2025_15a55280-en.html
10. USDA ERS — Food Security in the U.S.: Key Statistics (2024) — https://www.ers.usda.gov/topics/food-nutrition-assistance/food-security-in-the-us/key-statistics-graphics
11. FRAC — Hunger & Poverty in America (2024) — https://frac.org/hunger-poverty-america
12. OECD — Society at a Glance 2024: Income Poverty & Social Spending — https://www.oecd.org/en/publications/society-at-a-glance-2024_918d8db3-en/full-report/income-poverty_53d4eac1.html
13. WHO — Social Determinants of Health — https://www.who.int/news-room/fact-sheets/detail/social-determinants-of-health